When Should You Worry About High Blood Pressure? Understanding the Risks and Signs

(Note: Some of the links in this post are affiliate links, and we will be compensated when you make a purchase by clicking through our links at no additional cost to you.)
In the intricate symphony of our body’s functions, blood pressure emerges as the key conductor orchestrating the circulation of life itself. At its core, blood pressure embodies the force exerted by circulating blood against the walls of the arteries. This seemingly simple numerical measurement holds the answer to a crucial question: When should you worry about high blood pressure?
Imagine blood vessels as the highways of our circulatory system, and blood pressure as the traffic flow within. Just as controlled traffic maintains order on the roads, regulated blood pressure ensures the smooth transportation of oxygen and nutrients to every nook and cranny of our body. The measurement of blood pressure consists of two values: systolic pressure, the force when the heart beats, and diastolic pressure, the force when the heart rests between beats. The unit of measurement, millimeters of mercury (mmHg), reflects the pressure within the arteries.
Why does this matter? Well, maintaining a healthy blood pressure is akin to preserving the integrity of these circulatory highways. It’s the cornerstone of cardiovascular well-being. When blood pressure veers into the realm of hypertension, or high blood pressure, these once smoothly flowing highways can become turbulent waters, potentially leading to a cascade of health concerns.
The prevalence of high blood pressure is more than just a statistic; it’s a global health concern that silently affects millions. According to the World Health Organization (WHO), high blood pressure is responsible for nearly 10 million deaths worldwide each year. Its insidious nature lies in its ability to operate stealthily, often without overt symptoms, earning it the ominous moniker of “the silent killer.”
Table of Contents
Understanding Blood Pressure
When we speak of blood pressure, we are referring to the dynamic force exerted by the blood against the arterial walls as it courses through our circulatory system. This force is not uniform but is, in fact, a rhythmic interplay between two essential components: systolic and diastolic pressure.
Definition of Blood Pressure and its Components
Blood Pressure: It is the measure of the force exerted by circulating blood on the walls of arteries. Expressed in millimeters of mercury (mmHg), blood pressure is recorded as two values: systolic over diastolic. These values represent the peak force during a heartbeat (systolic) and the resting pressure between heartbeats (diastolic). For instance, a blood pressure reading of 120/80 mmHg indicates a systolic pressure of 120 and a diastolic pressure of 80.
Normal Blood Pressure Range and its Significance
Understanding the normal range is crucial in deciphering the language of blood pressure readings. A standard blood pressure reading falls within the range of 90/60 mmHg to 120/80 mmHg. The systolic value represents the pressure when the heart contracts, pumping blood into the arteries, while the diastolic value is the pressure when the heart relaxes between beats.
Importance of Maintaining a Healthy Blood Pressure for Overall Well-being
Maintaining a healthy blood pressure is not just a numerical target; it is a cornerstone of overall well-being. Think of it as the Goldilocks principle for cardiovascular health—not too high, not too low, but just right. Here’s why:
Cardiovascular Health: Optimal blood pressure ensures that the heart, our perpetual engine, works efficiently. It reduces the strain on the heart and lowers the risk of heart-related complications.
Circulatory Efficiency: Within the intricate network of arteries, veins, and capillaries, balanced blood pressure ensures a smooth flow of oxygen and nutrients to every cell and organ. This efficient circulation is vital for the body’s proper functioning.
Prevention of Complications: Maintaining a healthy blood pressure range significantly lowers the risk of serious health issues such as heart disease, stroke, and kidney problems. It is a proactive step towards safeguarding long-term health.
Identifying Hypertension:
When the blood pressure consistently measures at 130/80 mm Hg or higher, it falls into the hypertension category, marking a potential cause for concern. However, it’s essential to note that a single high reading does not automatically mean you have hypertension. Blood pressure can fluctuate throughout the day due to various factors such as stress, physical activity, or even caffeine intake.
Healthcare professionals employ a comprehensive approach to diagnose hypertension. Rather than relying on a solitary measurement, they prefer to consider multiple readings taken on different occasions. This approach helps account for the natural variations in blood pressure and ensures a more accurate assessment of your cardiovascular health.
The American College of Cardiology and the American Heart Association recommend monitoring blood pressure regularly, both at home and during clinical visits. Home blood pressure monitoring can provide valuable information about your blood pressure patterns in different settings, offering a more comprehensive picture of your overall cardiovascular health.
Moreover, healthcare providers may consider ambulatory blood pressure monitoring, a process where a portable device measures blood pressure at regular intervals over a 24-hour period. This method provides a more extended and detailed assessment, helping to identify any significant variations and ensuring a more precise diagnosis.
It’s important to understand that the diagnosis of hypertension involves not only the numerical values but also an evaluation of your overall health, lifestyle, and potential risk factors. If you receive a high blood pressure reading during a routine check-up, your healthcare professional may recommend additional tests, lifestyle modifications, or further monitoring before confirming a hypertension diagnosis.
Lifestyle and Risk Factors:
High blood pressure is often influenced by various lifestyle factors that, when left unaddressed, can significantly contribute to its development. Being mindful of these factors is crucial for both preventing and managing hypertension.
Dietary Choices:
A diet high in sodium and sugar is a known contributor to elevated blood pressure. Excessive salt intake can lead to fluid retention and increased strain on the heart. Similarly, a diet rich in refined sugars may contribute to obesity, a condition linked to hypertension. Adopting a heart-healthy diet, which includes fresh fruits, vegetables, whole grains, and lean proteins, can play a pivotal role in maintaining optimal blood pressure levels.
Physical Inactivity:
Lack of regular physical activity is a significant risk factor for high blood pressure. Engaging in regular exercise helps maintain a healthy weight, strengthens the cardiovascular system, and promotes overall well-being. Aim for at least 150 minutes of moderate-intensity exercise or 75 minutes of vigorous-intensity exercise per week to support cardiovascular health and reduce the risk of hypertension.
Tobacco Use:
Smoking is a well-established risk factor for hypertension and other cardiovascular diseases. The chemicals in tobacco smoke can damage blood vessels and elevate blood pressure. Quitting smoking not only benefits your heart health but also improves overall lung function and reduces the risk of other smoking-related diseases.
Alcohol Consumption:
Excessive alcohol intake can raise blood pressure and contribute to hypertension. While moderate alcohol consumption may have some cardiovascular benefits, it’s essential to be mindful of the quantity. For men, moderate drinking is generally defined as up to two drinks per day, while women are advised to limit intake to one drink per day.
Chronic Stress:
Chronic stress and its impact on blood pressure are interconnected. Prolonged stress can lead to increased heart rate and blood vessel constriction, contributing to hypertension. Adopting stress-management techniques such as meditation, deep breathing exercises, or engaging in hobbies can help mitigate the effects of stress on blood pressure.
If you engage in these behaviors or have risk factors such as a family history of hypertension, it becomes even more critical to monitor your blood pressure regularly. Home blood pressure monitors are readily available and provide a convenient way to track changes. By understanding the impact of lifestyle choices on blood pressure, you empower yourself to make informed decisions that can positively influence your cardiovascular health.
Health Conditions and High Blood Pressure:
Beyond lifestyle factors, certain underlying health conditions can significantly elevate the risk of developing high blood pressure. Recognizing these conditions and understanding their interplay with hypertension is essential for proactive health management.
Diabetes:
Individuals with diabetes are at an increased risk of developing high blood pressure. The two conditions often coexist in a phenomenon known as “diabetic hypertension.” Diabetes can damage blood vessels and the kidneys, leading to elevated blood pressure. Proper management of blood sugar levels through medication, diet, and lifestyle adjustments is crucial in preventing and controlling hypertension in individuals with diabetes.
Kidney Disease:
The kidneys play a vital role in regulating blood pressure by managing fluid balance and electrolytes. Kidney disease can disrupt this delicate balance, contributing to hypertension. Conversely, high blood pressure can also damage the kidneys over time, creating a dangerous cycle. Regular kidney function tests and monitoring blood pressure are essential for individuals with kidney disease or those at risk.
Genetic Predisposition:
Genetics can play a significant role in determining an individual’s susceptibility to high blood pressure. If there is a family history of hypertension, you may be more predisposed to the condition. Genetic factors can influence how the body regulates blood pressure and responds to various stimuli. While you cannot change your genetic makeup, awareness of familial predispositions can prompt proactive measures to manage other risk factors and adopt a heart-healthy lifestyle.
Regular health check-ups are instrumental in identifying these risk factors early on. Healthcare professionals can conduct routine screenings for conditions like diabetes and kidney disease, allowing for timely intervention and management. Additionally, understanding your family’s health history provides valuable insights that can guide personalized preventive strategies.
For individuals with a family history of hypertension or those diagnosed with diabetes or kidney disease, proactive blood pressure monitoring becomes even more critical. Regular check-ups, including blood pressure measurements and relevant diagnostic tests, enable healthcare providers to assess your cardiovascular health comprehensively.
>>> Read more: Discover the most accurate blood pressure monitor for home use. Click here.
Early detection and management of these underlying health conditions can not only help control high blood pressure but also mitigate the risk of complications associated with these diseases. It underscores the importance of a holistic approach to health, addressing both lifestyle factors and underlying health conditions to promote overall cardiovascular well-being.
When to Seek Medical Attention:
Monitoring your blood pressure regularly is a proactive step in maintaining cardiovascular health, but it’s equally important to be aware of certain signs and symptoms that may indicate a more urgent need for medical attention. If your blood pressure consistently measures above the normal range or if you experience specific warning signs, prompt intervention becomes crucial.
Consistently Elevated Blood Pressure:
If your blood pressure readings consistently measure above the normal range, especially if they persistently exceed 130/80 mm Hg, it’s a signal that your cardiovascular health may be at risk. While a single high reading may not be cause for immediate concern, persistent elevation warrants attention from healthcare professionals. Regular monitoring and consultation with your doctor can help identify patterns and determine appropriate interventions.
Symptoms of Hypertensive Crisis:
A hypertensive crisis occurs when blood pressure spikes to a dangerously high level, typically exceeding 180/120 mm Hg. This severe condition requires immediate medical attention. If you experience symptoms such as severe headaches, shortness of breath, chest pain, or visual changes, do not delay seeking help. These symptoms may indicate that your blood pressure has reached a critical point, posing an increased risk of organ damage or other complications.
It’s important to note that hypertensive crisis symptoms can be acute and severe, necessitating swift action. If you or someone around you exhibits these signs, call emergency services or seek urgent medical care without delay.
Understanding the Importance of the (>180/120) Threshold:
The specific threshold of (>180/120) signifies a level of blood pressure that requires immediate intervention. At this point, the risk of complications such as stroke, heart attack, or organ damage becomes significantly heightened. Seeking medical attention promptly is crucial in preventing or mitigating these severe consequences.
Healthcare professionals may administer appropriate medications or interventions to lower blood pressure rapidly in a controlled manner during a hypertensive crisis. This emphasizes the critical role of professional medical care in managing acute situations related to high blood pressure.
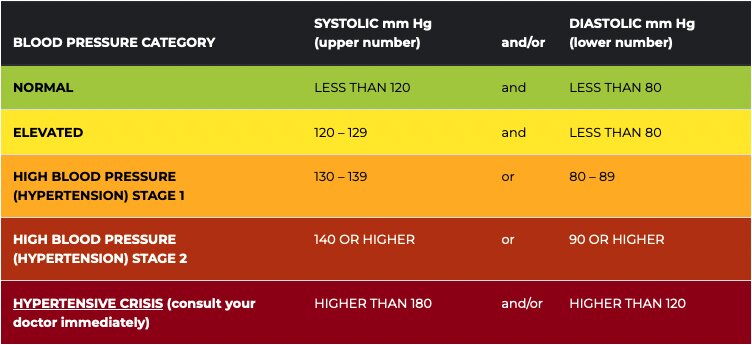
Image Credit: American Heart Association
Prevention and Management:
Maintaining optimal blood pressure is a lifelong commitment that requires a multifaceted approach, combining healthy lifestyle choices and, when necessary, medical interventions. Whether you’ve been diagnosed with high blood pressure or are proactively looking to prevent it, lifestyle modifications are at the forefront of effective management.
Heart-Healthy Diet:
Adopting a heart-healthy diet is a cornerstone of blood pressure prevention and management. The Dietary Approaches to Stop Hypertension (DASH) diet is specifically designed to lower blood pressure. This involves emphasizing fruits, vegetables, whole grains, lean proteins, and low-fat dairy while minimizing saturated fats, cholesterol, and sodium. Monitoring your salt intake is particularly crucial, as excess sodium can contribute to fluid retention and elevated blood pressure.
Regular Physical Activity:
Engaging in regular physical activity is a powerful tool in the prevention and management of high blood pressure. Regular exercise helps strengthen the heart, improve blood vessel function, and contribute to overall cardiovascular health. Aim for at least 150 minutes of moderate-intensity aerobic activity or 75 minutes of vigorous-intensity exercise per week. This can include activities such as brisk walking, jogging, swimming, or cycling.
Stress Management:
Chronic stress can contribute to elevated blood pressure, making stress management an integral part of blood pressure control. Incorporating stress-reducing practices into your daily routine, such as meditation, deep breathing exercises, yoga, or mindfulness, can help mitigate the impact of stress on your cardiovascular system. Finding activities that bring joy and relaxation is key to fostering overall well-being.
Tobacco Cessation:
Smoking is a significant risk factor for high blood pressure and cardiovascular diseases. Quitting smoking not only benefits your blood pressure but also improves lung health and reduces the risk of various other diseases. If you need support in quitting, consider seeking assistance from healthcare professionals or support groups dedicated to smoking cessation.
Moderate Alcohol Consumption:
While moderate alcohol consumption may have some cardiovascular benefits, excessive drinking can raise blood pressure. If you choose to consume alcohol, do so in moderation. For men, moderate drinking is generally defined as up to two drinks per day, and for women, limiting intake to one drink per day is recommended.
Regular Monitoring and Medical Check-ups:
Whether you’ve been diagnosed with high blood pressure or are actively working to prevent it, regular monitoring is essential. Home blood pressure monitors are valuable tools for tracking your progress. Additionally, scheduling regular check-ups with healthcare professionals allows for a comprehensive assessment of your cardiovascular health, enabling timely interventions if needed.
Medication Adherence:
In some cases, lifestyle modifications alone may not be sufficient to control blood pressure. If prescribed medication, it’s crucial to take it as directed by your healthcare provider. Adhering to the prescribed treatment plan ensures that your blood pressure remains within a healthy range and reduces the risk of complications associated with uncontrolled hypertension.
The only true way of ascertaining whether you have high blood pressure or not is by having it checked or monitored regularly using a home blood pressure monitor and tracking it with a blood pressure log. This is a painless procedure, and every adult should have their blood pressure checked regularly since your blood pressure can change over time. This way you are more likely to catch a change before it becomes dangerous. Ask your health care provider how often you need to check it.